An Executive Summary by Dr. Nick West, Abbott Vascular’s CMO
It’s sometimes difficult to explain the inner workings of a cardiac catheterization laboratory, even to those that work in healthcare outside of cardiac services; one analogy is that of a Formula One team’s pit stop: patients, akin to sophisticated racing cars, arrive in the cath lab with complex cardiovascular problems, and the role of the interventional cardiologists and the highly skilled team of specialized healthcare professionals is to run requisite diagnostics, analyze the issues, fix them with speed and precision in the least invasive way possible, so that they can continue their life journey. Whilst this is obviously a gross oversimplification, it does illustrate the role of the interventional cardiologist and team and the work they do in the cath lab – within the broader context of a complex and often disconnected network of healthcare providers and hospital administrators, where patients are expected to navigate and advocate for themselves.
So this is where the similarities between patient and racing car end. Patients often come to the cath lab with an extensive and complicated health history, with environmental, demographic and economic factors playing a role in determining overall health and well-being; regardless of diagnosis and treatment, it is an often-overlooked fact that these factors will follow them even after they leave the cath lab.
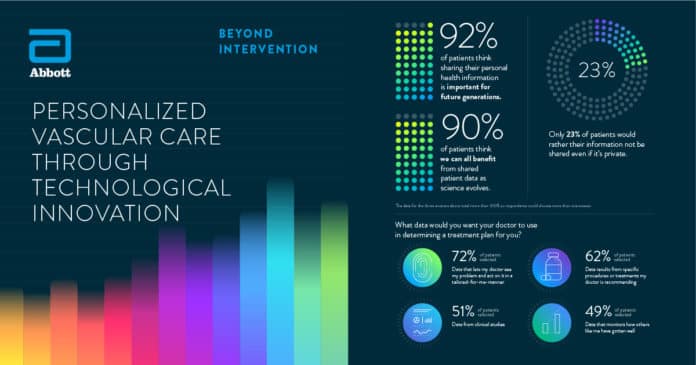
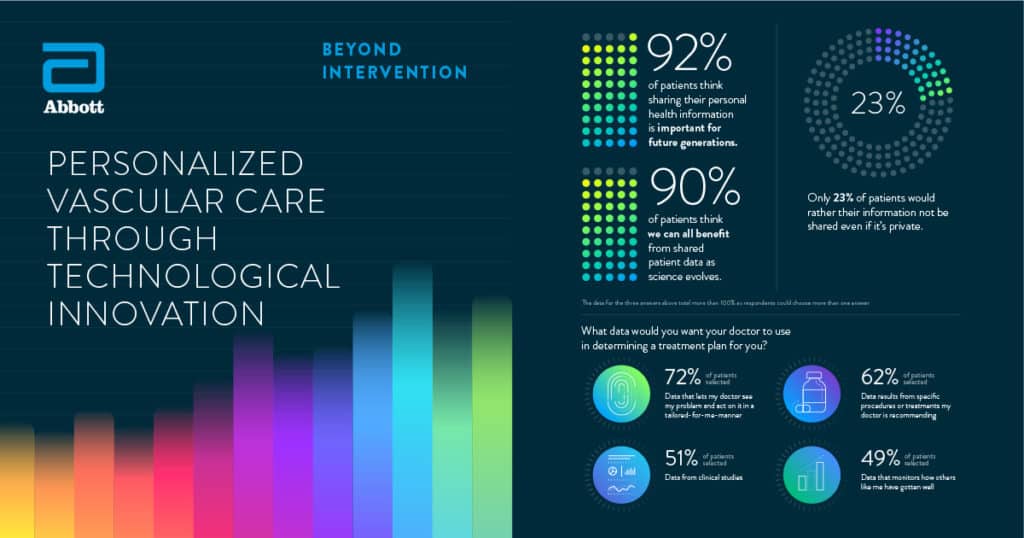
Given limited knowledge and understanding of the entire patient journey – or how patients arrive at the cath lab in the first place, and what happens after they leave – we undertook research to obtain a global view into the state of vascular disease care today, and gain insights into how cardiovascular treatments could be improved. Last year we surveyed 1,432 patients, physicians, and administrators, representing nine countries: the United States, the United Kingdom, China, Japan, France, Germany, India, Italy, and Brazil.
The results of the survey confirmed many issues that have personally experienced at first-hand as an interventional cardiologist: scarcity of time with patients, a lack of appropriate tools to aid with patients’ prescribed medication adherence and lifestyle changes, and disconnects/data gaps across the health care system. Such “black holes” in the care continuum leave physicians and administrators in the dark about their patients’ journey, and exemplify the fragmentation of existing health care systems across the world today. It is therefore absolutely no surprise that patients confirmed these observations, too, feeling that they lacked time with their physician and that subsequent personalization of care and treatment pathways remained suboptimal.
For more information – Cardiovascular.Abbott
Despite these frustrations, the majority of physicians and hospital administrators surveyed primarily d that advances in technology-driven diagnostics and treatments related to CVD in general have translated into tangible improvements in patient care, and can continue to do so if we can leverage the advances in healthcare informatics, big data analytics through artificial intelligence/machine learning and novel remote monitoring techniques.
On the surface, the results of the survey may appear discouraging, but in fact they demonstrate a mutual belief by all parties that effectively leveraging new technologies and patient data across the care continuum before, during, and after interventions has the potential to bring physicians closer to their patients, and to improve outcomes while remaining cost-effective.
Qualitative research like this provides a window into the world of cardiovascular disease care from differing perspectives, and I would encourage you to read the research: where the perspectives diverge and intersect are of equal importance – and by understanding what is happening at the physician level, the patient level and the hospital administrator level, we at Abbott are in a better position to meet the needs of those we aim to serve. Whether through life-saving medical devices or via supporting technologies, our goal remains the improving of outcomes for all vascular patients around the world.
It is now up to the medical device and technologies community, of which Abbott is a part, to take the initiative and act as the lynchpin between physicians, hospital administrators and patients, and to help develop a healthcare ecosystem that will benefit all stakeholders.