By Elise Copps
The practice of checking a patient’s pupils to determine how well their brain is functioning has existed for over 100 years. A nurse shines a light into the person’s eye and records how his or her pupils react, labeling them “brisk”, “sluggish” or “non-reactive”. It’s an important exam because it can give the health care team clues about brain activity and indicate whether urgent surgery might be necessary.
But this method is prone to human error. A variety of factors such as the brightness of the flashlight or varying perceptions of pupil size mean that results can be inconsistent. Small changes in reactivity may not be noticed until the brain is already in danger. To take the guesswork out of this process, Hamilton General Hospital (HGH) has adopted a new technology called a Pupillometer. HGH is one of only five hospitals in Canada using this device.
It’s manufactured by NeurOptics® and is officially known as the NPi™-200 Pupillometer. The device measures a number of factors including pupil size and reactivity, and can store up to 3,000 measurements in its internal memory bank. That allows trends and changes to be tracked over time.
Dr. Draga Jichici, a neurologist at HGH, says it will improve how quickly they can respond to small changes in a patient’s brain activity. “It will allow us to have an objective early warning sign that patients are deteriorating,” he says. “It will give us an opportunity to intervene before it worsens.”
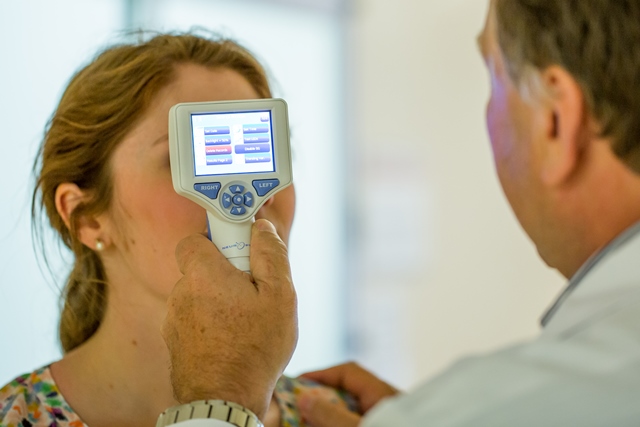
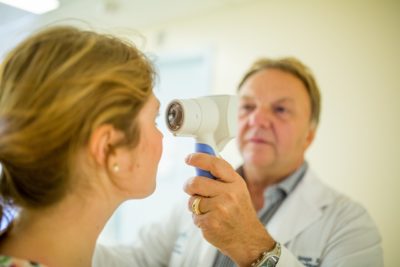
Instead of relying on the human eye to gauge reactivity, you point the Pupillometer at each pupil. Using infrared light, it records a video of the pupil and analyzes it to decide how reactive it is. The Pupillometer measures several factors including the speed at which the pupil dilates, its size at maximum dilation and the delay between the onset of light stimulation and pupil reaction. All of these variables are combined and measured against a normative scale to produce a rating on the Neurological Pupil index™.
Instead of using subjective terms like “sluggish” and “brisk,” the Pupillometer’s measurement index gives a rating from 0-5. A score of 3 or greater indicates a normal reaction. 1 or 2 indicates that the pupil is less reactive than normal and a score of 0 means it isn’t responsive at all. Used alone, each individual score can help the patient’s care team decide whether to stay the course of treatment or attempt a new intervention. Combined over time, they can provide even greater insight.
The thousands of scores that are potentially stored in the device can be charted to visualize changes in responsiveness. A clinician using the device can see how pupil size and reactiveness has evolved in recent hours, days or even weeks. The visual map is a clearer indication of small changes that could warrant urgent action, such as surgery to relieve pressure on the brain.
The objective scoring system also allows clinicians to identify plateaus over time. If a patient’s pupils consistently score 0, the reality that they are not improving may solidify earlier than if that responsiveness was being measured subjectively by the naked eye.
The Pupillometer can also connect to an electronic medical record so the patient’s ratings can be tracked in their chart and viewed alongside other important indicators. The ability to easily track changes based on the numeric rating scale will help clinicians to develop the best plan of action for that patient. In some cases, this could mean the difference between life and death.
“The pupil’s changes can precede life threatening changes for the patient,” says Dr. Jichici. “These changes may indicate that we need to check the patient more frequently, order certain tests or perform emergency surgery on the brain.”
The Pupillometer is already in use in the Neurosciences Unit at HGH and is in the process of being introduced to the hospital’s Intensive Care Units. Keisha Jack is the clinic manager of the Neurosurgery and Neuromodulation Program at HGH and was involved in creating a protocol for ordering the test and phasing in the device.
It has become an important tool in making connections between clinical and neurological findings. She says staff has responded well to the technology and feels more confident when performing neurological exams using the Pupillometer rather than the naked eye. “Clinicians appreciate the objectivity the Pupillometer provides,” says Jack. “It allows for more accurate assessments and reporting of changes in the clinical status of the patient. That translates into timely interventions, appropriate clinical decision making and better outcomes.”
Elise Copps works in Public Relations & Communication at Hamilton Health Sciences.