By Carla Peacock
Living with a chronic illness like Chronic Obstructive Pulmonary Disease (COPD) used to mean frequent visits to the emergency department and long hospital stays resulting from acute flare-ups. But thanks to new vital signs monitoring technology, patients can monitor the status of their condition daily to help identify and prevent potential emergency situations.
Markham Stouffville Hospital (MSH) in partnership with Women’s College Hospital (WCH) Closing the Gap Healthcare and Cloud Diagnostics Canada (Cloud Dx) developed a comprehensive self-management program that includes a connected health kit and personalized action plan for COPD patients. They can use this program to be more knowledgeable about their disease and recognize when they require additional interventions. This will shorten the impact of a flare-up and reduce the impact that it has on their recovery and quality of life.
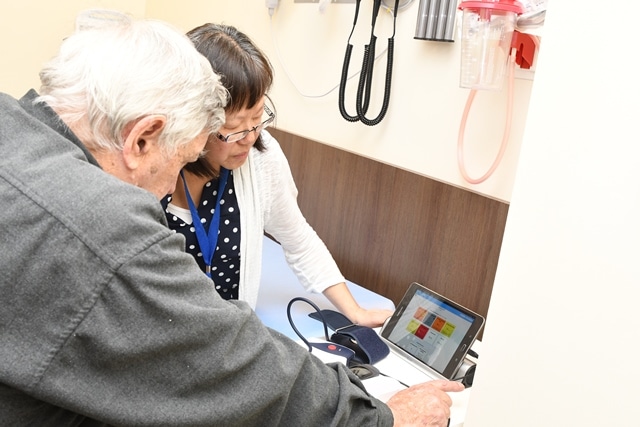
The connected health kit allows patients to measure and record their own vital signs and quantify their breathing capacity using blood pressure, oxygen saturation and COPD assessment scores. When patient specific predetermined thresholds are met, automated notifications are sent to the patient and a healthcare provider. Using a tablet or other wireless devices accompanied with a patient specific action plan, patients are better able to self-manage their condition at home and avoid crises moments.
“I used to guess about when I should worry about my symptoms. But now that has changed, by recording my own vital signs, I know what’s going on and if I need to take my additional medication to avoid flare-ups,” says John Grabiec of Stouffville, who has been living with COPD for over 20 years. Grabiec has found the Cloud DX technology has been easy to use. It has reduced his visits to the hospital and given him peace of mind that his care team is monitoring his symptoms as well.
Three little words: Using text messages to support adherence
“We know more about our patients’ symptoms and we can prevent serious flare-ups so that they don’t have to come into the hospital,” says Sheery Tse, Respiratory Therapist. “With this technology, patients work with care providers to keep themselves healthy and living independently.”
In addition, WCH is leading a research study to investigate the effectiveness of this technology by comparing the current standard of care to both a technology enabled self-monitoring program and a technology enabled combined self- and remote monitoring program for this patient population. The effectiveness of this program will be measured by examining patients’ self-management skills, quality of life, COPD knowledge and respiratory symptoms. Secondary outcomes include tracking ED visits, hospital admissions, and length of stay for COPD patients.
“The study is in its early stages but we have already seen great success with our rapid pilot project. One of our patients reported avoiding a visit to the emergency department by monitoring their vitals and following their action plan over a long weekend when the clinic was closed,” says Katrina Engel, Respiratory Therapist and Clinical project Specialist at MSH.
This technology was made possible with funding from Ontario’s Health Technologies Fund (HTF). The fund is administered by Ontario Centres of Excellence (OCE) on behalf of the Office of the Chief Health Innovation Strategist (OCHIS), and is a part of the OCHIS mandate to strengthen Ontario’s health innovation ecosystem.
This project is one of 12 MSH SmartCare innovations that the MSH Transformation Office has launched in the past year. Combined, these projects have impacted the lives of over 1,300 people. For MSH, ‘SmartCare’ describes innovations and tools that support a culture of innovation. It’s about providing care to patients in a way that is more efficient, more convenient, better coordinated, and smarter.
Partnerships have been essential in developing this culture of innovation, and achieving success. MSH has been fortunate in building great partnerships to explore new innovative healthcare delivery models that achieve better outcomes, better experience, and greater efficiency for our patients, staff, and physicians.
Carla Peacock is a Senior Communications Specialist at Markham Stouffville Hospital.
