More than 14,000 people have received medical assistance in dying (MAID) in Canada, since it was legalized in 2016. Although organ donation is an option for only a fraction of this population, healthcare teams and researchers are working in innovations and new protocols to respect these patients’ final wishes while also allowing for them to help those in need of a transplant.
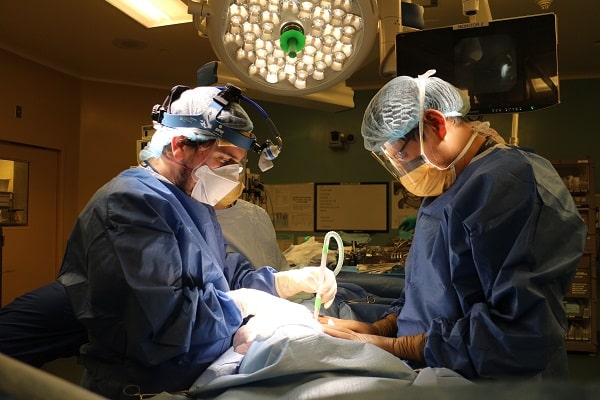
In a coordinated effort with Trillium Gift of Life Network (TGLN), the organization in charge of organ and tissue donation in Ontario, the Toronto Lung Transplant Program at UHN’s Ajmera Transplant Centre has performed the first transplant surgery after MAID at home.
“This is ground-breaking as it allows for us to respect the donor’s wishes while also paving an important new avenue to save lives,” says Dr. Marcelo Cypel, Surgical Director at the Ajmera Transplant Centre and corresponding author of the scientific paper reporting this case.
The case happened thanks to the great generosity of Sergeant Mike Neill, who received MAID at his home in Burlington, Ont., after a long battle with Huntington’s disease.
“In our experience in Ontario, a significant portion of MAID patients who are eligible to donate organs value dying at home more than donating organs and this is critically important to respect,” explains TGLN’s Chief Medical Officer for Donation, Dr. Andrew Healey.
“Our combined expertise and most current protocols allow us to respect these patients’ end-of-life plan while also honouring their incredible generosity in giving the gift of life.”
This world-first was possible thanks to Sergeant Neill’s generosity and because of an innovative protocol in place for lung transplantation in Toronto – the result of a collaboration between UHN, TGLN, William Osler Health System, and air ambulance and medical transport service, Ornge.
Non-Perfused Organ Donation
Since 2016, UHN’s Ajmera Transplant Centre has been able to perform lung transplants from deceased donors who had not previously been on life support. Known as Non-Perfused Organ Donation (NPOD), this protocol allows for lungs to be preserved for a longer period of time after an unexpected death – such as a heart attack – and still be suitable for transplant.
Lungs are unique organs in that they can stay viable even after a couple of hours without blood circulation in the donors’ body, as long as they are full of air explains,” Dr. Cypel. “So we implemented a strategy to reinflate the organ after death declaration and family authorization.”
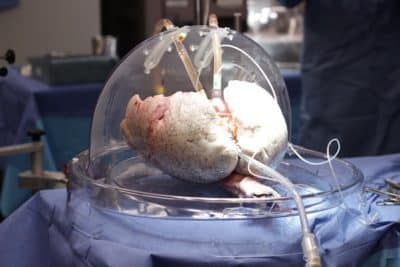
Because in these cases there is no time to evaluate the organ function in the donor, the NPOD protocol is only possible thanks to Ex Vivo Lung Perfusion (EVLP) system, a landmark advance in lung transplantation pioneered by Drs. Cypel and Shaf Keshavjee, Director of the Toronto Lung Transplant Program and of the Latner Thoracic Research Laboratories.
“We are in a unique position in the world to lead this innovation as we have the technology and the partnerships to implement the necessary protocols,” Dr. Cypel says.
UHN’s Ajmera Transplant Centre also had the support from the donor hospital and medical transport teams. Joseph Brant Hospital in Burlington performed the donor surgery and the lungs were transported by Ornge to Toronto General Hospital (TGH).
“The success of this case is the result of a concerted effort by a number of teams,” says Dr. Jonathan Yeung, thoracic surgeon who did the recipient surgery at TGH, and Senior Author of the scientific paper.
The patient who received the transplanted lungs suffered from end-stage lung disease.
By the end of 2019, there were more than 230 patients waiting for a lung transplant in Canada alone, and the estimate is that 20 per cent of patients die while waiting for lungs to become available.
Find out how to register to become an organ or tissue donor at BeADonor.ca.
This article was submitted by University Health Network.
