By Brenda Wilson, Wendy Levinson and Jennifer Young
October is breast cancer awareness month and information about screening can be confusing. Who should have a screening mammogram and at what age? What are the benefits? Are there any downsides? People deserve clear information when it comes to breast cancer screening.
But there’s no single answer to any of these important questions since personal health history and patient preferences and values are a critical part of the decision-making process. Breast cancer screening decisions require a conversation with your health provider — this is called shared decision making.
This year, we expect to see over 28,000 people develop breast cancer in Canada, and 5,500 will die. The good news is that with more effective treatments, the outlook has improved for those diagnosed with breast cancer. Screening can help detect the cancer before it gets too advanced.
What does breast screening involve?
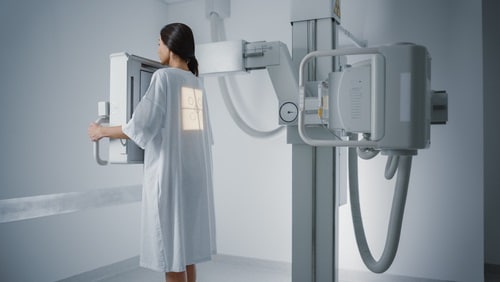
Breast cancer screening includes checking breasts for signs of cancer before there are symptoms of the disease. This can be done through a specialized x-ray called a mammogram.
As groups that provide guidance to primary care providers — family doctors, nurse practitioners and other health care professionals — we try to provide clarity on mammography screening as another way to possibly reduce the risk of dying from breast cancer.
So, what’s the most recent advice?In 2018, the Canadian Task Force on Preventive Health Care published a guideline about breast cancer screening for average risk individuals aged 40-74. The guideline aims to help people understand both the benefits and harms of screening, and provide recommendations based on best evidence. Simply put, starting at the age of 40, it’s always a person’s choice to get screened or not based on personal preferences and discussions with their trusted health care provider.
In creating these guidelines, the Task Force always includes patients’ values and preferences around screening. The guideline does not apply to those at increased risk of breast cancer, including individuals with a personal or strong family history of breast cancer or those who are carriers of gene mutations. Breast cancer risk goes up with age: the older a person, the more likely it is the benefits of screening will outweigh the harms, up to the age of 74.
In Canada, provinces and territories have different recommended age ranges for when they start breast cancer screening. For example, while some provinces recommend screening at 40, other provinces recommend screening should start at 50.
So why not just have a mammogram? Isn’t screening obviously good?
Not always. At the very least, screening can lead to a false positive, which is a test that is positive when there is not really disease. This can cause unwanted anxiety and further unnecessary investigations. It can also lead to more invasive tests like biopsies. And science tells us that not all early cancers actually progress, as we used to think. For some people, this means life changing treatments that were never necessary, and sometimes complications that were not inevitable.
It can be helpful to visualize the benefits and harms of breast cancer screening, so the Task Force has created a number of resources that can help patients and health care providers have the conversation: https://canadiantaskforce.ca/tools-resources/breast-cancer-update/.
With new scientific research, knowledge of the harms and benefits of screening evolves. So, every five years, the Task Force reviews its guidelines to provide new information and updates. The mammography guideline will be up for review in 2023.
But right now, the guidance stands: if a person prefers to have a mammogram, they should have a mammogram guided by an informed conversation with their health care provider.
Brenda Wilson is Co-Chair of the Canadian Task Force on Preventive Health Care.
Wendy Levinson is the Chair of Choosing Wisely Canada.
Jennifer Young is a Physician Advisor for the College of Family Physicians of Canada.