By Andria Bianchi
At the time of writing this column, most Canadians will likely be familiar with Coronavirus disease 19 (COVID-19). As defined by the World Health Organization (WHO), “[c]oronaviruses (CoV) are a large family of viruses that cause illness ranging from the common cold to more severe diseases such as…Severe Acute Respiratory Syndrome (SARS-CoV).” These viruses are zoonotic, which means that they spread from animals to humans (WHO 2020).
COVID-19 is a new coronavirus strain that emerged in China and has never been identified in humans before. The WHO labelled the COVID-19 outbreak a global health emergency in January 2020, and more recently classified it as a pandemic. As of March 11, over 118,000 cases have been identified across 114 countries. In an attempt to contain the virus, individuals are being encouraged to maintain social distancing, avoid unnecessary international travel, etc.
In a public health crisis such as that of COVID-19, many questions need to be answered in order to help society deal with its implications. For instance, what exactly is COVID-19? (How) can we contain it? Can we cure it? Who is most vulnerable? Do travel bans actually work to stop it from spreading?
In addition to consulting with experts to help us answer important descriptive and clinical questions such as those noted above, it is also the case that ethicists are often consulted in public health crises.
Although one may not immediately think of ethicists as important contributors to consult with during a pandemic, there are many complex ethical questions that need to be responded to in a timely, thoughtful, and well-reasoned manner during these situations. I will highlight some of these questions below. It is impossible to adequately respond to the questions in this short column since a response would also require providing information about thorough decision-making frameworks developed by ethicists.
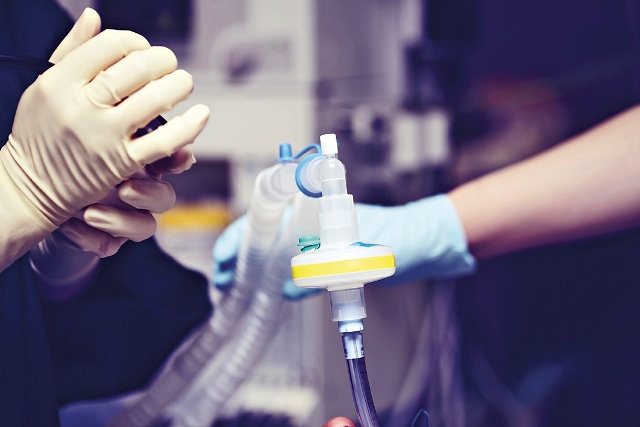
Some of the most cited and difficult dilemmas that occur in a pandemic are those regarding the prioritization and dissemination of scarce resources. For instance, if multiple people test positive for COVID-19 and require a ventilator/an isolated room/a treatment in order to survive, yet there are only a few ventilators/rooms/treatments available, then who ought to be prioritized? Should we prioritize the person who is most likely to make a full recovery? The taxpaying citizen? The person who is the youngest? The philanthropist? Etc. Ultimately, who ought to die and who ought to survive? Making decisions about how to prioritize scarce resources during a pandemic requires the careful consideration of multiple competing values, which is precisely what ethicists are trained to do.
Alongside questions of resource allocation, there are also often questions asked about whether and under what conditions healthcare workers are obliged to care for patients in an outbreak. Are there certain conditions under which it may be ethically defensible for healthcare workers to not attend work (even if they offer an essential service to patients)? If so, what might those conditions look like?
Other questions that exist extend beyond hospital walls. For instance, at what point might it be defensible to place restrictions on individual citizens’ freedoms (e.g. via travel bans, city lockdowns, etc.)? Given the importance placed on autonomy (particularly in Western liberal societies), the decision to limit an individual’s right to engage/not engage in certain activities ought to be taken seriously.
Finally, what are our obligations to society’s most vulnerable, such as those who depend on our shelter system? As a result of COVID-19, many shelters will be closed for the foreseeable future. And while a decision to close shelters would not have been made lightly, it is worth highlighting the cost that this decision will have on some of society’s most vulnerable and unsupported people. From the perspective of justice, it seems reasonable to suggest that we owe these individuals a great deal of resources and support in response to the COVID-19 outbreak (which may lead us to also ask: where should these resources be taken from? And to whom ought they be given if they are scarce in number?).
Ultimately, there are many ethical dilemmas that arise during an outbreak that require thoughtful attention. Ethicists working at hospitals, within community settings, and in partnership with organizations such as Toronto’s Joint Centre for Bioethics (JCB) are trained to respond to these complex questions. They are an essential part of a pandemic planning and response team.
Here are some resources developed by the Joint Centre of Bioethics in response to the novel coronavirus pandemic: https://jcb.utoronto.ca/news/covid-19.shtml.
Andria Bianchi, PhD, is a Bioethicist and Clinician-Scientist at the University Health Network and an Assistant Professor at the Dalla Lana School of Public Health- University of Toronto.