Cardiac surgeons at St. Michael’s Hospital have successfully treated a rare congenital heart anomaly using minimally invasive cardiac robotics — marking a landmark achievement in cardiac surgery.
In late November, Drs. Gianluigi Bisleri and Daniel Burns treated a patient with a rare congenital condition known as cor triatriatum. This anomaly is characterized by a thin membrane within either the left or right atrium, dividing the chamber into two compartments. As a result, patients effectively have three atrial chambers instead of two, which restricts blood flow and can lead to shortness of breath, fatigue, and even heart failure.
The case comes just months after St. Michael’s became the first hospital in Toronto to implement a robotic platform in cardiac surgery and perform a robotic mitral valve repair. Building on that momentum, Drs. Bisleri and Burns applied their advanced expertise to an even more complex condition, which they say is the first-ever robotic surgical treatment of cor triatriatum worldwide.
With robotics, highly trained surgeons are able to operate through small incisions, resulting in shorter hospital stays, reduced risk of infection, and significantly faster recovery compared with traditional open-heart surgery.
Tackling complex cases with robotics
The Schroeder BRAIN&HEART Centre is one of Canada’s highest-volume cardiac centres, with a strategic focus on expanding its robotic program to address rare and highly complex cardiac conditions — bringing the benefits of advanced technology to more patients.
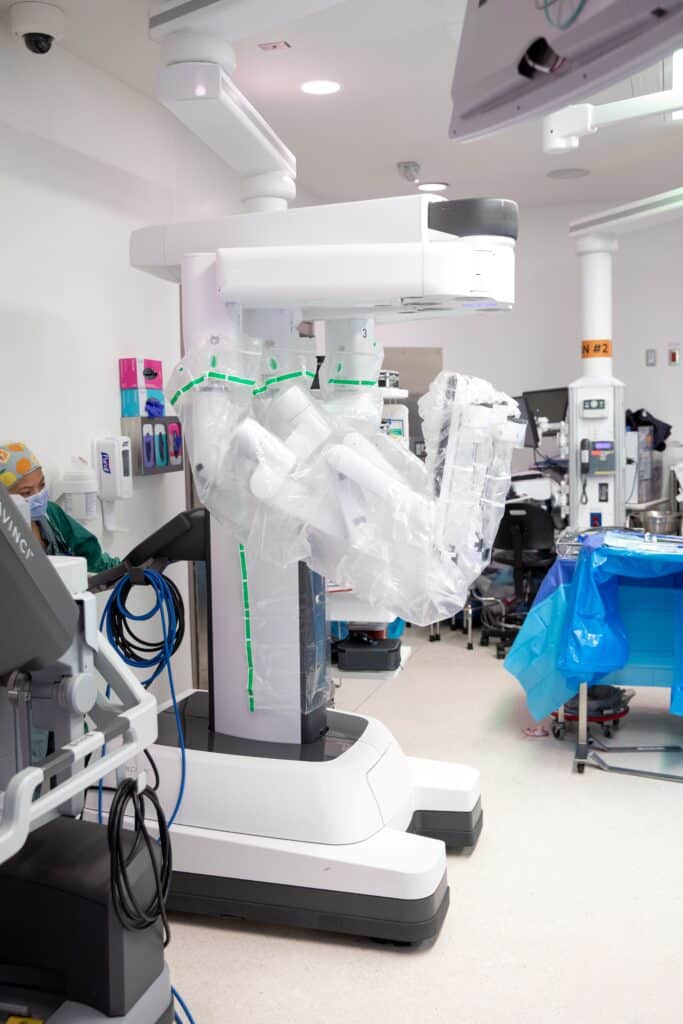
The da Vinci system has two main components: the endoscope, or the “eyes,” and three robotic arms, each equipped with an EndoWrist that replicates — and enhances — the surgeon’s natural hand movements. This added range of motion allows surgeons to perform intricate maneuvers in confined spaces with exceptional precision.
The system’s high-definition, three-dimensional endoscopic visualization is a critical advantage. While cardiac surgeons traditionally rely on magnifying loupes, the robotic platform provides unparalleled clarity—essential in this case to ensure complete and precise removal of the abnormal membrane from the patient’s heart chamber.
Unlike conventional open-heart surgery, which requires splitting the breastbone and lengthy recovery, robotic cardiac surgery often allows patients to return home within a few days.
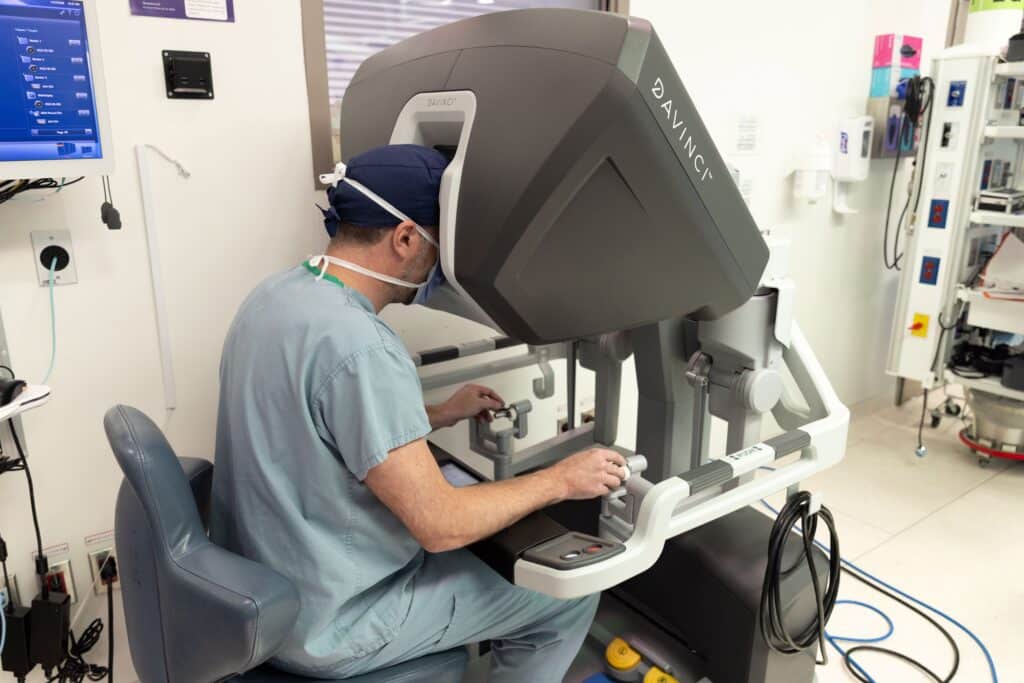
During the procedure, Bisleri and Burns worked in close coordination. The da Vinci system is controlled from a nearby console, where the surgeon views a magnified three-dimensional image of the surgical field and uses hand and finger controls to perform delicate, highly precise movements.


Innovative and advanced care for all
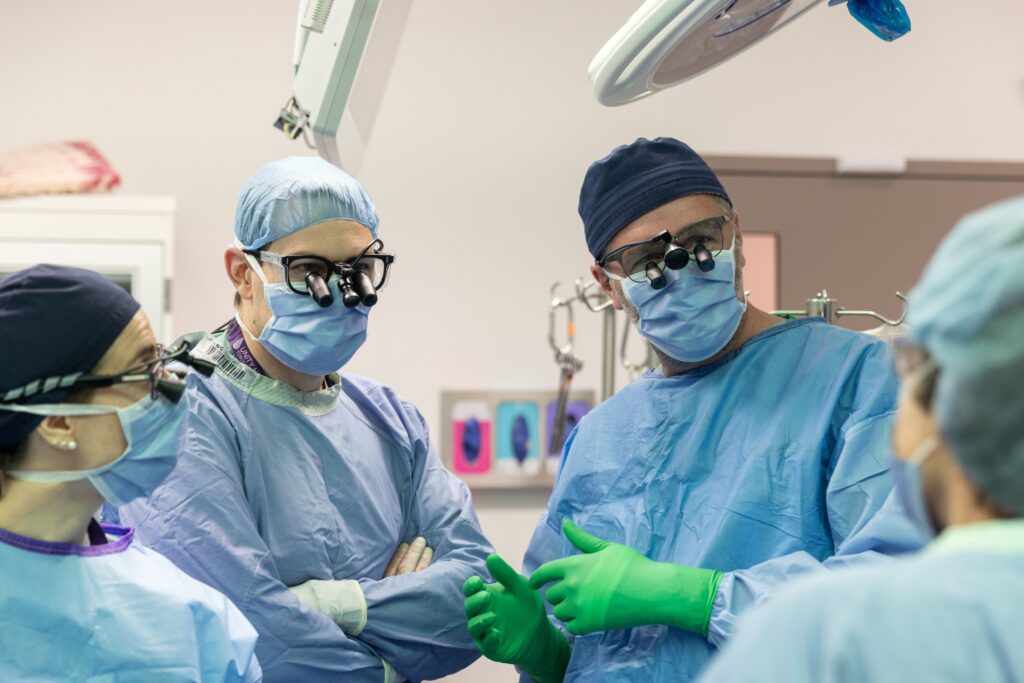
This progress in care is possible because of the highly skilled surgeons who can operate the powerful robotic tools, and the anesthesiologists, nurses, and perfusionists who are driving this innovative and patient-centred practice forward. “The successes never stop,” says Altaf Stationwala, President and CEO of Unity Health Toronto. “I am very proud of this team. We’re fundamentally changing how heart surgery is done, but also changing access to care.”
Following the three-hour surgery, the patient was discharged from hospital after three days and is recovering well at home. Robotic surgery is a significant step forward for patient care and recovery, with so much potential for new ways to help patients heal and return to their regular lives.
“We are fortunate that irrespective of where you come from, we all have access to the most significant and impactful care,” says Stationwala. “And we’re very fortunate that our clinicians continue to push the envelope and make people’s lives that much better.”
By Christine Davidson
Photos by Katie Cooper

