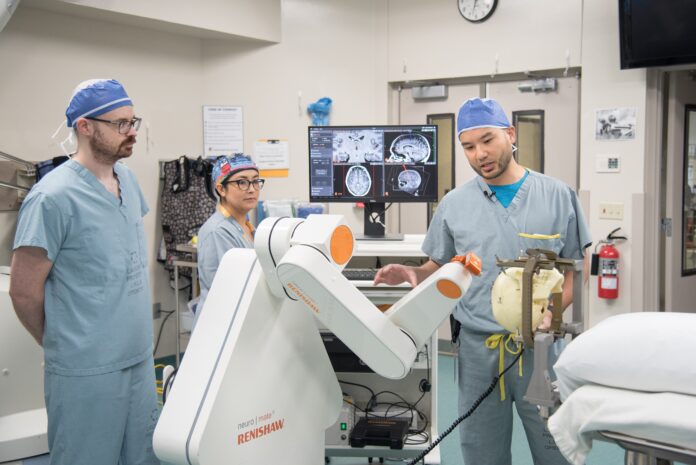
First Canadian robot-assisted deep brain stimulation surgery to treat epilepsy successfully completed at LHSC’s University Hospital
For the first time in Canada, a robot-assisted deep brain stimulation surgery to treat seizures caused by epilepsy was successfully completed at the London Health Sciences Centre’s (LHSC) University Hospital (UH).
Deep brain stimulation surgery involves placing electrodes in the brain that are connected to a pacemaker which provides stimulation to alter brain activity enough to prevent or limit seizures.
Using the Renishaw neuromate® robot to assist in the surgery enables accurate and safe placement of electrodes while accessing difficult to reach areas of the brain. “The robot allows accurate, individualized trajectories and can quickly move between electrode implants with minimal manual intervention,” said Dr. Jonathan Lau, who has successfully completed three surgeries using the robot since January. “This is a significant development that provides a new option using a surgical robot for accurately placing brain pacemaker electrodes across a wide range of neurological disorders.”
Epilepsy is characterized by recurrent seizures, which are brief episodes of involuntary movement that may involve a part of the body (partial) or the entire body (generalized) and are sometimes accompanied by loss of consciousness. It is one of the most common neurological disorders in the world and affects an estimated 300,000 Canadians.
Sometimes epilepsy can be treated by removing the part of the brain where the seizures originate but if it is an area that is responsible for an essential activity such as logical thinking or a more generalized process, removing the area is not an option.
That is where deep brain stimulation can come in and Dr. Lau is the first surgeon to use a robot to assist in this specific surgery in Canada to treat the condition. “It’s a treatment that’s available to patients who were traditionally not considered candidates for surgery,” explains Dr. David Steven, a neurosurgeon at UH and Chair of the Department of Clinical Neurological Sciences at the Schulich School of Medicine and Dentistry at Western University.
Acquired in 2017 though a donation to London Health Sciences Foundation (LHSF), the neuromate® was first used in robotic-assisted stereoelectroencephalography (SEEG) procedures which map epileptic seizure activity in the brain for patients whose complex epilepsy may not respond to medication or traditional treatment. Dr. Lau has taken it a step further to treat the condition and change the lives of those who can experience up to dozens of seizures a day.
This year marks the UH’s 50th year of serving the community and the region and it continues delivering world-class, cutting-edge care, says Cathy Vandersluis, president of UH. The advancement achieved by Dr. Lau and his team is just the most recent in the field of neurosurgery.
“Since we first opened our doors in 1972, we’ve had a long history of breaking ground in surgical techniques, including in neurosurgery,” she says. “It started with Dr. Charles Drake in 1972 when he began operating on brain aneurysms using a technique that established the University Hospital’s worldwide reputation in the field of neurology, and it continues today.”
For Drs. Lau and Steven, it is all about helping more patients.
“By the time we see them, the seizures, or the fact that they might have a seizure, gets in the way of their everyday life,” says Dr. Steven, “and additional medications or changing medications rarely is successful. For some patients, this is an extremely effective treatment and reduces their seizures by a very significant amount.”