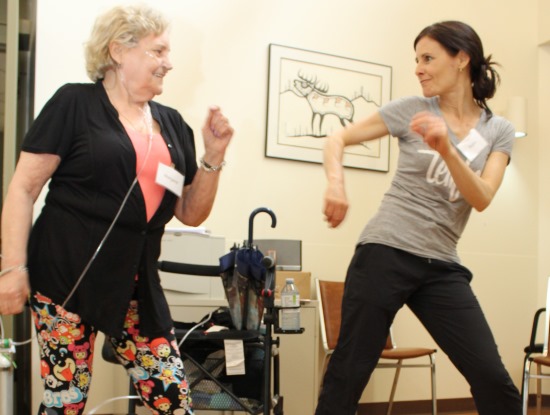By Jane Langille
After showing significant improvement by participating in a formal rehabilitation program, many people living with chronic obstructive pulmonary disease (COPD) find it difficult to maintain their progress when the program ends.
A unique feasibility study at West Park is investigating the effectiveness of dancing to music to help people with COPD sustain or improve their level of physical activity post-rehabilitation. COPD is a group of lung diseases that include chronic bronchitis and emphysema, and is the third leading killer of men and women in the world. There is no cure for COPD and it gets worse over time. But with access to rehab, you can slow its progress and improve your quality of life.
“I have been working with stroke patients using dance, so it made sense to see if it might help people living with COPD,” says Dr. Dina Brooks, a Senior Scientist who has been performing research at West Park for over 20 years. “Dance is fun and social. Patients prefer it to exercise on a treadmill or going for a walk. It is also an excellent way to address balance issues, which affect many of these individuals.” Dr. Brooks is also a professor in the Department of Physical Therapy at the University of Toronto.
STUDY GOALS
As a result of West Park’s expertise in respiratory rehabilitation, it treats the most COPD inpatient rehab cases of any healthcare centre in the province. Dr. Brooks is collaborating on this research together with Dr. Roger Goldstein, West Park’s Director of Respiratory Medicine and Dr. Kara Patterson, an assistant professor in the Department of Physical Therapy at the University of Toronto.
In the study, two groups of 10 participants meet for a 1-hour dance session twice a week for eight weeks. Participants boogie to a variety of different dance styles tailored to their preferences, including tango, contemporary, salsa and cha-cha. They can dance with a class partner or on their own, as they desire. A trained dance instructor with experience working with people with chronic illnesses leads the sessions.
“We are measuring the impact of dance on physical activity, balance, quality of life, life satisfaction, and levels of anxiety and depression,” says Dr. Brooks. “We are also tracking participants’ heart rates with Fitbit activity bands, to see if they are getting a good workout.”
The study began in April and will extend over the summer. Participants are over the age of 40 and have completed a course of pulmonary rehabilitation at least four months in advance of the dance program.
Dr. Brooks has authored or co-authored dozens of studies while at West Park. She currently focuses on research involving individuals with chronic lung disease and those with cardiovascular disease. She is a Canada Research Chair (Tier 2) in Rehabilitation Chronic Obstructive Pulmonary Disease and the recipient of several teaching and research awards and research grants.
RESEARCH AWARD
This study, which is officially called “Let’s Boogie: feasibility of dance in patients with chronic obstructive pulmonary disease,” is supported by a Breathing as One – Boehringer Ingelheim Canada COPD Catalyst Grant from the Canadian Lung Association. The researchers plan to report on the study results in the fall of 2017.
“Learning from this research will inform the program design for a larger, randomized controlled trial in the future,” says Dr. Brooks. “From the smiles and sense of comfort and level of engagement we’ve seen so far in the first group, we hope to confirm that dance intervention can make a meaningful difference in physical fitness, balance, quality of life, anxiety and depression. We think dance may turn out to be an excellent way to help more people with COPD continue to realize their potential.”
Jane Langille is a freelance Toronto writer