By Selma Al-Samarrai
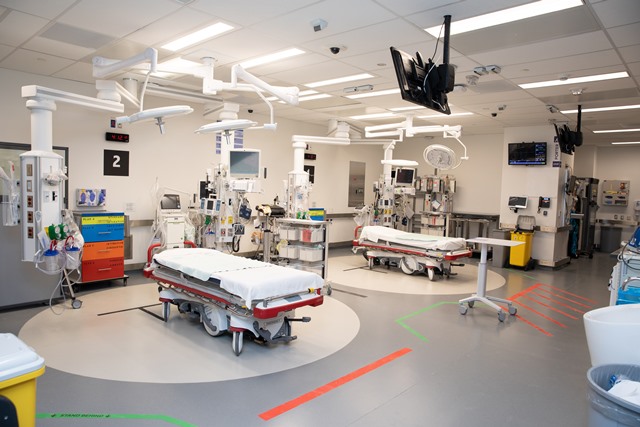
A brand new trauma bay has opened inside St. Michael’s Hospital’s Slaight Family Emergency Department (ED) after a lengthy and carefully planned testing and design process that ensured trauma patients will get the best possible care when they need it most.
“No patient should ever be the first test of a new trauma care space; that’s a key principle behind the design of our new trauma bay,” explains Dr. Andrew Petrosoniak, Emergency Physician and Trauma Team Leader at St. Michael’s Hospital and Unity Health Toronto’s Clinical Integration and Translational Simulation Lead.
“We believe that we should simulate scenarios as a means to test the equipment and the space, ensuring that it works as we imagine it will. We do this so that by the time we open for patient care, we’ll know that all systems are a go.”
As a Level 1 adult trauma centre, St. Michael’s cares for an average of 1,100 patients in its trauma bay per year, with the number increasing by 18 per cent between 2015 and 2019. The trauma bay is a specialized care area where patients with traumatic, life-threatening injuries are rushed to upon arriving at the ED.
The Operational Readiness, led by Dominic Gascon, Operational Readiness Specialist, and Margaret Moy Lum-Kwong, Senior Director of Operational Readiness, and the ED and trauma teams began partnering on the design of the new trauma bay back in 2017.
“Two of the key principles in operational readiness are patient safety and staff safety. It’s not ideal to build a space without understanding exactly what happens in the space, and how patients and clinicians flow through it,” explains Moy Lum-Kwong.
“So rather than looking back and seeing how we used to do it, we told the trauma team to look forward and ask: how should we do it?”
The teams used various simulation techniques to optimize the design of the space, conducting different exercises in a phased timeline so learnings from one test could be applied to the next.

It started with table-top simulations 18 months before the construction of the trauma bay even began. A large group from the ED and trauma teams — including nurses, doctors, respiratory therapists, clerical staff and clinical assistants — all gathered around a massive blueprint of the new space to visualize it and test the flow of staff in the room using cotton balls to represent patients and staff.
Next came the mock-up simulation: the Operational Readiness team built a replica trauma bay and asked the trauma team to run a full-scale simulation in it.
“The blueprints provided in the table-top simulations are valuable at an early stage but the difference between them and the mock-up simulation is the latter really allows you to figure out the details that can only be determined when you’re inside the space, such as the best position for the vital signs monitor where it can be seen by the entire team,” explains Dr. Petrosoniak.
Finally, they conducted in-situ simulations inside the almost completed trauma bay. The team ran six completely different medical scenarios over the course of two days so that they could finalize key details such as floor markings to guide where individual team members should stand and planned locations of life-saving equipment so that they can be quickly accessed.
“In situ simulation is the last stop – it confirms that our designs and early simulation work resulted in the most streamlined way of delivering care to critically injured patients. When we need immediate, life-saving interventions, we expect that the equipment will be at our fingertips and that we’ll have the necessary space to make that easy. A well-designed workspace is absolutely critical when seconds matter, and we’re excited that we’ve achieved that,” says Dr. Petrosoniak.
A key resource used in the design of the trauma bay was the findings of the 2016 TRUST study, conducted by Dr. Petrosoniak and Dr. Chris Hicks, fellow St. Michael’s Emergency Physician and Trauma Team leader. The year-long study, supported by the Allan Waters Family Simulation Centre, both observed and inquired about how trauma team members interact with one another and with the space to see what changes they could implement to make the trauma bay more conducive to efficient and collaborative patient care.
“St. Michael’s is really ahead of the curve for integrating the clinical team in the design of the space the way they did. We’re grateful for the Operational Readiness team’s safety-minded approach and that we have a simulation program that can support this type of work,” says Dr. Petrosoniak.
Selma Al-Samarrai is a communications advisor at Unity Health Toronto.