By Sarah Garland
You probably know someone who snores. And their snoring may be pretty loud and disruptive. Maybe it’s so disruptive that it’s causing their bed partner — or even those in the next room — to toss and turn. But it’s possible that it’s more than just snoring. They could have a disorder called obstructive sleep apnea (OSA), a condition in which the muscles of the upper airway collapse during sleep, causing their breathing to stop and start. Although OSA is reported to affect around 15% of men and 5% of women in Canada, the true prevalence may be as high as one in four adults, with many people going undiagnosed. Not everyone with OSA snores, but it is a common symptom. People with OSA may also experience unrefreshing sleep and excessive daytime sleepiness, as well as impaired memory and concentration. It’s hard to overstate the importance of sleep, especially a good night’s sleep; and if left untreated, OSA can lead to stroke, cardiovascular disease, hypertension, diabetes, motor vehicle accidents, cognitive dysfunction, and death.
To diagnose OSA, patients are often sent to sleep overnight in a sleep lab, or in some cases technology is available to diagnose OSA in a patient’s own home. Some people may be diagnosed with mild OSA, while OSA in others may be moderate or even severe. One way to measure the severity of OSA is to use the apnea-hypopnea index (AHI), which looks at how often a person stops breathing and how often their breathing becomes very slow and shallow. Typically, AHI scores of 5 to 14 are considered mild OSA, scores of 15 to 29 are considered moderate OSA, and scores of 30 or more are considered severe OSA. A person’s AHI score and OSA severity can help patients and their health care providers make decisions about treatment.
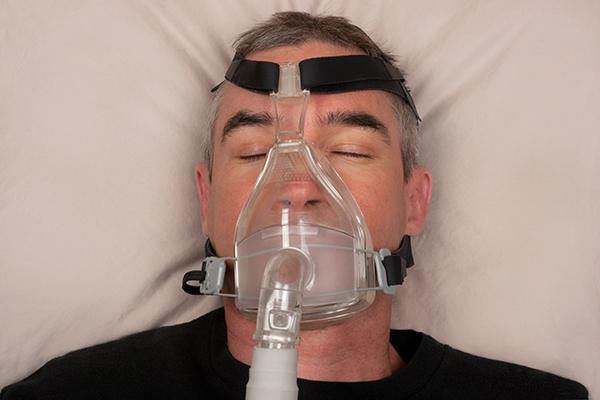
What are the options for treating OSA? In Canada, there are a number of ways to treat this sleep disorder. Continuous positive airway pressure (CPAP) devices, which work by forcing air into the upper airway to keep it open, are often considered the gold standard for treatment. There are also other positive airway pressure (PAP) devices that work in slightly different ways, like auto-titrating PAP, bilevel PAP and nasal expiratory PAP (disposable devices that use a patient’s own breath to open up the airway). In addition to PAP devices, there are oral appliances, which work by moving the jaw forward or by holding the tongue back to create space and keep the airway open. Beyond devices, there are surgeries for OSA, the most common being maxillomandibular advancement (MMA), which permanently moves the jaw forward. For adults who are overweight or obese — a risk factor for OSA — other interventions, like diet and exercise, focus on weight loss, which can improve OSA symptoms.
With so many treatment options, how do you choose the right one? An important consideration is whether a person will actually use their OSA treatment. Though some consider CPAP the best option for treating OSA, it’s estimated that 29% to 83% of patients don’t use their device regularly as recommended. And it’s not really clear how many patients actually use their oral appliance to treat their OSA. The evidence around how well surgery works to treat OSA and whether it’s safe is also uncertain. There is also the question of whether patients will have to pay out of pocket for their OSA treatment or whether reimbursement and funding of these different treatment options is available to them. Public coverage for CPAP varies by province, and no provincial programs reimburse oral appliances. Surgery may be covered, if available.
To help address the choice of treatment for adults with OSA, CADTH — an independent agency that finds, assesses, and summarizes the research on drugs, medical devices, tests, and procedures — conducted an evidence review on the different options for treating OSA. The CADTH report assessed the clinical and cost-effectiveness, safety, and patient and caregiver perspectives and experiences related to the various treatment options for OSA in adults. Ethical issues, implementation considerations, and potential environmental impacts were also addressed. An expert panel, the Health Technology Expert Review Panel (HTERP), reviewed the evidence and developed recommendations for treating OSA.
The review of the clinical evidence found that all of the treatment options for OSA are effective at reducing excessive daytime sleepiness and the severity of OSA. However, people with severe OSA may benefit more from CPAP than oral appliances. The cost-effectiveness of the treatment options varies by OSA severity. The review also revealed that using the treatments for OSA require people to adapt their daily routines and relationships, and that some people are able to integrate the treatment into their life and experience benefits, while others are unable to do so.
Based on the evidence review, three key recommendations by HTERP emerged. The first being that lifestyle interventions (like diet and exercise) are recommended for adults with mild OSA if they are overweight or obese. For those with mild OSA who are not overweight or obese, no treatment is recommended. The second recommendation is that for adults with moderate or severe OSA, CPAP is recommended; but if the person cannot tolerate CPAP or CPAP is unacceptable, then oral appliances are recommended. Lastly, surgery was not recommended, unless other interventions have failed or are unacceptable to the patient.
CADTH’s work, and the recommendations by HTERP, highlight the importance of adapting treatment to a patient’s OSA severity and other patient factors. People may prefer or be better suited to one treatment over another for a variety of reasons, including coverage and reimbursement for the costs of the various treatments, access to dentists and dental health specialists for oral appliances, access to electricity to power CPAP machines, and potential side effects and discomfort experienced from any of the treatments.
So what does all this mean to people with OSA, their families, and their health care providers? There are effective options when it comes to treating OSA. And CADTH evidence can help guide those treatment decisions.
To learn more, visit www.cadth.ca/OSA or speak to a CADTH Liaison Officer in your region.
Sarah Garland is a Knowledge Mobilization Officer at CADTH.