By Marc LePage
Since the first human genome was sequenced in the early 2000s, genomics – the science that aims to decipher and understand the entire genetic information of an organism – has had immeasurable impacts in the health sector. Genomics is now driving a revolution in precision health – an approach that is increasingly employed in health-care settings and stands to improve the lives of millions of Canadians.
For generations in Newfoundland and Labrador, seemingly healthy young men were struck by a mysterious affliction that would appear suddenly and kill them in their 20s and 30s. They would, quite literally and inexplicably, drop dead of sudden cardiac arrest.
This remarkable phenomenon prompted a team at Memorial University in St. John’s to investigate a possible genetic explanation for what had been dubbed colloquially a “family curse.” With support from Genome Canada and Genome Atlantic, researchers identified and profiled affected families and, in February 2008, published the news that they had isolated the gene responsible for arrhythmogenic right ventricular cardiomyopathy (ARVC).
Today, a simple blood test can diagnose ARVC and patients with the genetic mutation are preventively implanted with a defibrillator. To date, more than 160 people in Newfoundland and Labrador have been successfully treated as a result of this genetic testing. Other ARVC patients have also been fitted with defibrillators in mainland Canada, the United States, Denmark, Germany, Spain, Norway, and in other countries around the globe, preventing countless heart attacks and adding some 30+ years to the lifespan of individuals who receive the device.
This is just one example of how medicine is being transformed by genomics and precision health. Precision health is an approach that enables diagnosis and treatment to be tailored based on a patient’s unique genetic makeup. Given that genetic differences can explain why some people respond well to certain treatments while others do not, doing this systematically in health care can be transformative.
As anyone knows who has watched a television medical drama – from Marcus Welby M.D. to House – the practice of medicine is usually a variation on the classic detective procedural. A patient presents mysterious symptoms, the doctor evaluates the evidence against suspected culprits and a hopeful course of action is adopted. Now, genomics – in combination with big data, predictive analytics and other areas of cutting-edge science and technology — is enabling trained professionals to significantly telescope the process of elimination, solving diagnostic mysteries at the genetic level with far greater speed and efficiency, while producing more accurate answers.
Internationally, there is a sense of excitement about what this means for the future of medicine. The government of Canada, through funding for Genome Canada, has been at the forefront of what is now a collegial global competition to harness the transformative power of genomics toward more efficient, effective and economical health care.
To this end, the federal government, Genome Canada, and partners announced a $255 million investment in genomics and precision health research this January, bringing new hope for Canadians living with cancer, cystic fibrosis, juvenile arthritis, childhood asthma and other diseases. The results of Genome Canada’s 2017 Genomics and Precision Health competition, announced by federal Minister of Science Kirsty Duncan, includes a $162 million investment through Genome Canada, the Canadian Institutes of Health Research (CIHR) and co-funding provinces and partners in 15 genomics and precision health projects across Canada, in addition to $93 million for 10 genomics technology platforms across Canada.
One of these projects is UCAN CURE: Precision decisions for childhood arthritis, led by Drs. Rae Yeung (The Hospital for Sick Children) and Susanne Benseler (University of Calgary). More than 24,000 children in Canada live with painful, chronic arthritis. With the help of powerful drugs called biologics, doctors can dramatically reduce joint inflammation and pain and prevent long-term joint damage. But first, doctors must determine — using the first genomics-based, low-cost biomarker blood test — who needs biologics, which biologic will work best for an individual child, and when the biologic can be safely stopped.
One of the children who may benefit from UCAN CURE attended the precision health announcement with Minister Duncan at SickKids in Toronto. Aida Kelf-Kowal is nine years old and was diagnosed at age five with juvenile idiopathic arthritis. She and her parents went through an overwhelming process of trial-and-error before finally finding a medication that put her arthritis into remission. UCAN CURE will reduce this diagnostic odyssey and help make sure kids like Aida receive the best and most appropriate medication available as quickly as possible.
These breakthroughs require collaboration at the policy level so that innovations in genomic science and precision health are not stymied by the challenges of implementation. In October 2016, Genome Canada, the six regional Genome Centres and CIHR co-hosted a Genomics and Precision Health Forum in Toronto, where stakeholders, experts and opinion leaders from Canada and around the world compared notes on the implementation of genomics in their health-care systems.
Among the valuable takeaways from the event was the consensus that the major challenges in bringing precision health to clinical settings are generally policy-related rather than technical. The speed of genomic sequencing is now fast and cost is dropping — but major challenges exist around data sharing, privacy, infrastructure and other legal and ethical obstacles to implementation. We are working hard with public and private partners to overcome these challenges comprehensively and responsibly.
That forum laid the groundwork for a precision health strategy in Canada with specific recommendations:
- Develop a national vision for the implementation of genomics into the health-care system and start with a demonstration project in a targeted area to provide the foundation for precision health more broadly.
- Incorporate a health technology assessment service in publicly funded research projects to ensure a harmonized and proactive pathway for the assessment of new technologies.
- Establish national guidelines for the assessment and evaluation of genomic tests to support a harmonized and streamlined approach to the adoption of genomic tests by each province.
- Develop and promote the adoption of national standards for the collection, aggregation, integration, storage and governance of data generated with public sector funds, in alignment with the standards articulated by the Global Alliance for Genomics and Health.
- Support the development of appropriate curriculum and tools for the education and training of students and health-care practitioners to ensure the comprehensive and equitable use of genomic tests in clinical care.
- Consider how elements established by Canada’s Strategy for Patient-Oriented Research and related initiatives and platforms can be integrated into existing health-care delivery and research structures.
- Develop a white paper to articulate the roles and responsibilities of each stakeholder involved in health-care system transformation and help strengthen the precision health research and delivery continuum.
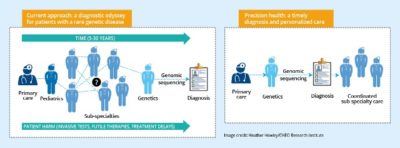
Genome Canada is contributing to a national effort on precision health in numerous ways, including spearheading a demonstration program focused on patients with rare genetic disease — a group of approximately one million Canadians, more than 50 per cent of whom are children. This initiative builds on several past and current projects and is designed to tackle questions of governance frameworks, data standards and more.
Our focus on rare diseases will help develop the infrastructure, skills, experience and partnerships essential for the implementation of a nationally harmonized program that leverages Canada’s burgeoning reputation as a global leader in pediatric precision health. Incidentally, Dr. Brendan Wren — one of Britain’s leading experts on the genomics of infectious and tropical diseases and a member of Genomics and Precision Health competition international peer review committee — said of Canada’s research excellence in the field, “If I were ill, particularly if I had a sick child, I would want to live in Canada rather than anywhere in the world.”
The promise of precision health is a future where the best health care available meets personal needs with improved outcomes and strong economic growth for Canada. This country has the political will to drive innovation in health-care delivery, including an increasing focus at the provincial level, a thriving genomics research culture, an ethnically diverse population and a universal health care system that make us exceptionally well-placed to advance the precision health revolution. That vision will require leveraging our world-class knowledge and expertise, capitalizing on the unique assets of the Canadian health-care system and genomics enterprise, and ensuring genomic-based innovations can be effectively implemented for the benefit of people here and the world over.
Marc LePage is President and CEO of Genome Canada.

