By Caitlin Johannesson
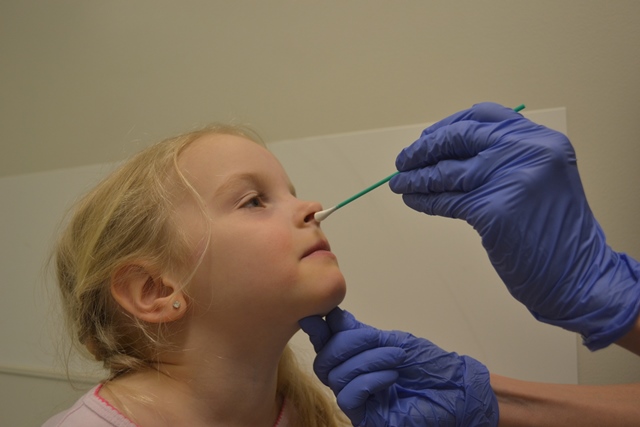
In 2014, more than 2,000 kids who visited SickKids Emergency Department with respiratory symptoms were given an invasive and uncomfortable nasopharyngeal swab test. This is when a doctor or nurse inserts a long swab into the nostril to the back part of the nose to collect a sample of cells. The swabs are sent to the lab to test for six common respiratory viruses, but the results come back the next day, often after patients have already been discharged from the Emergency Department. With no set process for communicating positive or negative results for this test, the results generally did not impact the child’s care.
With an increased emphasis on ‘choosing wisely’ and reducing unnecessary medical tests and therapies across the medical field, paediatricians at The Hospital for Sick Children (SickKids) say it is not good enough to ‘do’ these tests just because we ‘can’. The team examined the benefits and limitations for this specific type of test and reviewed the scientific evidence as to when it is actually helpful in improving patient care. The review, including their recommendations, was published in the July 3 advance online edition of JAMA Pediatrics.
Most viral respiratory illnesses can be diagnosed clinically based on the child’s symptoms (for example, runny nose, cough, nasal and chest congestion), but with more sophisticated and sensitive tests available, frontline clinicians frequently order tests to identify the specific offending virus.
“While the number of testing options has grown rapidly, the same attention has not been given to deciding how and when these tests can add value to the care of our patients. Just because the test is available, doesn’t mean we should automatically order one, especially since we know that for the majority of healthy children the result will have no impact on their care,” says Dr. Jeremy Friedman, senior investigator of the review and Associate Paediatrician-in-Chief at SickKids.
The review describes some of the common rationale used to justify respiratory viral testing but found poor evidence to support these rationales. Unsupported rationale includes:
- to reduce the number of lab blood tests and chest x-rays performed, as well as unnecessary antibiotic use
- to reduce the length of hospital stay
- to offer prognostic information on length of the illness, and a confirmed diagnostic label for the physician and the family
- to reduce healthcare costs
The team emphasized that there are clinical scenarios where respiratory viral testing can inform treatment decisions and improve overall patient care and therefore should be seriously considered. These examples include children with compromised immune systems, those at risk for influenza-related complications, children admitted to intensive care units, and infants with fever younger than three months old.
“We hope this review helps health care providers make better decisions and think twice before ‘checking the box’ for a nasopharyngeal swab on the list of possible investigations,” Dr. Peter Gill, lead author of the review and senior paediatric resident at SickKids.
As part of SickKids Choosing Wisely initiatives, SickKids has reduced nasopharyngeal testing for typical respiratory viruses in the Emergency Department by greater than 80 per cent since 2014.
This paper is an example of how SickKids is contributing to making Ontario Healthier, Wealthier and Smarter. www.healthwealthiersmarter.ca
Caitlin Johannesson is a communications officer at The Hospital for Sick Children.